UNSW researchers awarded $33m for medical research
Fifteen projects have received funding from the Australian Government's Medical Research Future Fund.
Fifteen projects have received funding from the Australian Government's Medical Research Future Fund.
Yolande Hutchinson
UNSW Sydney External Engagement
0420 845 023
y.hutchinson@unsw.edu.au
UNSW Sydney researchers have been awarded over $33 million under the Australian Government’s Medical Research Future Fund (MRFF), with projects spanning chronic lower back pain, childhood dementia, cervical cancer and more. The MRFF helps Australia’s medical researchers discover new ways to diagnose, treat and care for people with a variety of health conditions. They also support early and mid-career researchers and give more Australians access to clinical trials.
Scientia Professor Vlado Perkovic, Dean of UNSW Medicine & Health and Acting Provost - Faculties, congratulated the academics on receiving grants.
“I’m extremely proud of my colleagues who have received grants in this round of MRFF funding. The projects cover a broad range of medical issues from RNA vaccines to the treatment of depression. I look forward to seeing the outcomes of the projects which will undoubtedly have a positive impact on many Australians,” Prof. Perkovic said.
A Kirby Institute-led consortium that will boost development of RNA vaccines and therapeutics for COVID-19 and other health threats in Australia has received $5 million.
“The COVID-19 pandemic brought about rapid advances in mRNA and RNA development, and we saw particular success with the mRNA vaccines against COVID-19, demonstrating significant potential of RNA technology as a tool against other health threats,” says Kirby Institute Director Scientia Professor Anthony Kelleher, who is chief investigator on the project. “We welcome this funding from the MRFF, which will enable us to harness and scale up RNA technology in Australia.”
The consortium, Bringing RNA Innovations through the Developmental Gap Effectively, or BRIDGE, is an academic industry partnership, linking the Kirby Institute, Medicines Development for Global Health, Scientia Clinical Trial Research, the Garvan Institute for Medical Research, UNSW RNA Institute, along with community representatives on the Clinical Development Advisory Committee.
Independently, these institutions are leaders in RNA and drug development. BRIDGE will leverage this existing expertise and infrastructure to collaboratively boost innovation, rigorously assess potential products, and progress mRNA vaccines and RNA therapeutics from preclinical development through to first-in-human and early phase clinical trials.
The partnership will also facilitate greater access to RNA vaccines and therapeutics for low- and middle-income countries through enabling licensing of successful products through Medicines Development for Global Health so that they can be manufactured and distributed cost-effectively.
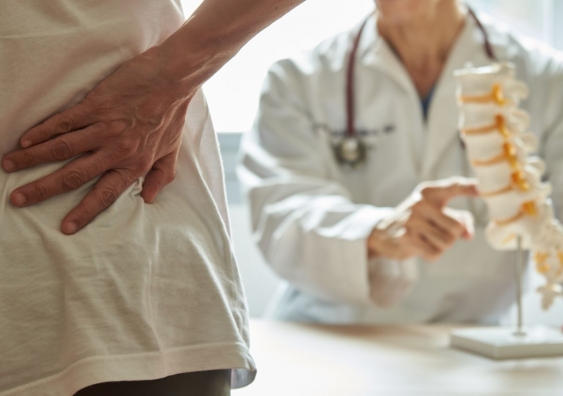
Professor James McAuley, along with Professor Sylvia Gustin, Dr Aidan Cashin and Dr Rodrigo Rizzo from NeuRA and UNSW Medicine & Health have been awarded a $1.6 million grant to test the effectiveness and best-practise implementation of a prescribable mobile app for chronic low back pain in primary care.
“Low back pain is the most prevalent musculoskeletal condition and has been the leading cause of long-term disability globally for 30 years. In Australia, chronic low back pain is very common, disabling and costly,” said Prof McAuley.
“In this trial we’re aiming to reduce pain and disability of people with chronic low back pain by empowering them with access to the best possible information and health tools no matter where they live in Australia. We’re also looking to inform the development of future digital interventions for the management of chronic disease.”
Professor Claire Vajdic from The Kirby Institute and UNSW Medicine & Health has received over $1.58 million to build a new health equity digital navigation tool that will fast-track the elimination of cervical cancer in Australia.
“This project addresses a major health problem in Australia, which is the urgent need for targeted cervical cancer prevention services in primary care for disadvantaged populations,” Prof. Vajdic said.
“There is a huge amount of existing health and social data in Australia. What this project will do is bring this data together, so we can rapidly identify gaps and overlooked areas that require more attention to achieve cervical cancer elimination.”
Prof. Vajdic said there are five priority population groups who experience barriers to prevention services: people with a disability, Aboriginal and Torres Strait Islander peoples, people with socioeconomic disadvantage, people from culturally and linguistically diverse backgrounds, and people living in remote areas.
Professor Michelle Farrar and a research team including Postdoctoral Fellow Dr Arlene D’Silva from UNSW Medicine & Health received $595,955 for a project that will monitor clinical trials in childhood dementias.
“Childhood dementias result in neurocognitive decline, progressive loss of skills and behavioural changes, all of which have a devastating impact. It is imperative that therapies for childhood dementia are investigated so that effective treatments are developed for this devastating condition,” Prof. Farrar said.
The Biomarkers to trEAT Child Dementia (BEAT CD) study will establish ways to measure neuroinflammation, oxidative stress, metabolic dysfunction and neurodegeneration across multiple childhood dementia disorders.
The study will provide measures for diagnosis, prognosis and evaluating effects of potential therapies. BEAT CD will streamline the pipeline from preclinical studies to clinical trials, increase opportunities for the development and implementation of multiple therapeutics.
The other UNSW projects to receive funding are:
Dr Jordana McLoone from the School of Clinical Medicine at UNSW Medicine & Health has received $4.7 million for a project that aims to optimise the transition from paediatric to adult healthcare services.
Professor Jane Butler from NeuRA and UNSW Medicine & Health has received $2.99 million for a project that will investigate neurostimulation to improve walking after spinal cord injury.
Associate Professor Natalie Taylor and her team from the School of Public Health & Community Medicine have received $2.99 million for targeted, adaptive genomics for ethical, evidence-based expansion of newborn screening: a type II hybrid effectiveness-implementation trial.
Professor Colleen Loo from the School of Psychiatry at UNSW Medicine & Health has received $2.98 million for a project that will investigate the comparative effectiveness of ketamine and esketamine in the treatment of resistant depression.
Professor Jason Grebely from the Kirby Institute at UNSW Medicine & Health has received $2.06 million for a project that will enhance point-of-care testing for hepatitis C infection.
Professor Gail Matthews from the Kirby Institute and UNSW Medicine & Health has received $1.99 million for a project that will investigate strategies and treatments for respiratory infections and viral emergencies.
Professor Christine Jenkins from The George Institute for Global Health and UNSW Medicine & Health has received $1.87 million for the Breathlessness Rapid Evaluation And THErapy (BREATHE) Project.
Associate Professor Jodie Ingles from the Garvan Institute of Medical Research and UNSW Medicine & Health has received $1.49 million for a study into using genomics to diagnose and manage inherited cardiovascular diseases.
Dr Matthew Jones from the School of Medical Sciences at UNSW Medicine & Health has received $1.38 million for a telehealth, effectiveness-implementation hybrid trial to increase physical activity in adults with chronic low back pain.
Dr Adam Hill from the Victor Chang Cardiac Research Institute and UNSW Medicine & Health has received $968,000 for a project investigating bioengineered tissue models to identify new antiarrhythmics for atrial fibrillation.
Dr Ira Deveson from the Garvan Institute of Medical Research and UNSW Medicine & Health has received $954,000 for a project that will harness nanopore sequencing technology to improve diagnosis of human disease.