The search for a malaria vaccine
Our battle with malaria disease has lasted thousands of years. We need better vaccines or we risk losing, according to UNSW Sydney researchers.
Our battle with malaria disease has lasted thousands of years. We need better vaccines or we risk losing, according to UNSW Sydney researchers.
Maddie Massy-Westropp
UNSW Medicine & Health
m.massywestropp@unsw.edu.au
Malaria is among the oldest of human diseases. There are traces of Plasmodium, the parasite that causes malaria, in ancient Egyptian mummies. Some records say that Alexander the Great died in 323 BCE from malaria.
“It’s clearly a very ancient pathogen,” said Professor Jake Baum, who leads a team of malaria researchers at UNSW Medicine & Health.
Yet, malaria is still a major threat to over half of the global population. The disease kills more than 600,000 people every year, most of these being children under five.
The first malaria vaccine took over 50 years to develop before being licensed in October 2021. It is only 30-40 per cent effective at preventing malaria – a far cry from the COVID-19 vaccines that were also licensed in 2021, after less than 12 months of development.
“We’ve been involved in a very longstanding arms race with malaria. The parasite and humans have been trying to outwit each other,” Prof. Baum said.
“I think the parasite is winning at the moment.”
Malaria is a disease caused by the Plasmodium parasite, which is transmitted between humans by Anopheles mosquitoes. When a mosquito bites an infected person, it takes in blood containing microscopic Plasmodium parasites. Later when the mosquito moves onto another person for its next blood meal, parasites mix with the mosquito’s saliva and are injected into the person being bitten.
“I like to describe the spread of malaria as a relay race. It’s a baton that is passed between us and a mosquito,” Prof. Baum said.
Read more: Of cats and crocs: new study on bites in the tropics reveals which animals are biting us
People with malaria typically become very sick with high fevers, shaking chills and flu-like illness. This can progress to seizures, brain damage, trouble breathing, organ failure and death.
Malaria is very treatable with antimalarial drugs but delays in diagnosis and treatment can have serious consequences. This is particularly an issue for people living in, or travelling to, disadvantaged areas with less access to quality healthcare.
“Malaria doesn't need to kill anybody. But it does,” Prof. Baum said.

Professor Jake Baum leads the Baum Lab's efforts to develop an effective malaria vaccine. Photo: UNSW.
Malaria poses a risk to people in tropical and subtropical areas, including sub-Saharan Africa, Asia, South America and Central America.
“Malaria can be transmitted wherever the Anopheles mosquito is present. So anywhere with enough moisture, and a warm enough temperature,” said Dr Michael Johnson, a member of the Baum Lab at UNSW Medicine & Health.
People outside of these areas, including Australians, typically have a lower awareness of malaria. However, the danger is still present.
“Human impacts on the environment can certainly have an impact on parasitic diseases like malaria,” Dr Johnson said.
For example, in Malaysia some humans have been infected with strains of malaria previously found only in monkeys. This is thought to be related to the destruction of monkey forest habitats and increasing contact between monkeys and humans. Also, due to climate change, the territory and biting behaviour of the Anopheles mosquito could change.
“We have no malaria here in Australia. But we certainly have the Anopheles mosquito here in Northern Australia,” Dr Johnson said. “And so it is definitely possible that localized epidemics could occur in the future.”
Vaccine development has been difficult for several reasons, one being that the Plasmodium parasite has a complex life cycle. The parasite takes on many different forms when it infects and breeds inside of a human host, presenting a shifting target for a vaccine.
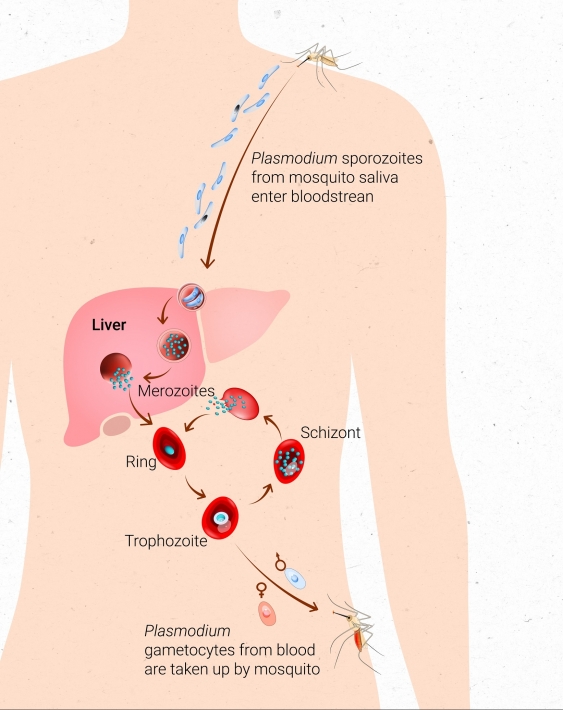
The Plasmodium parasite has a complex life cycle, taking on different forms when if infects and replicates inside of a human host. Image: Ian Joson.
When GlaxoSmithKline’s Mosquirix vaccine was licensed in 2021, this was a historic moment, but the vaccine was still only 30-40 per cent effective with rapidly waning immunity. Other candidate vaccines are in development, including the highly anticipated R21/Matrix-M vaccine, but the lack of a lasting immune response is still an issue.
“We need a much better vaccine if we’re really going to entertain the idea of getting rid of malaria, which is the driving ambition of many, including myself,” Prof. Baum said.
The Baum lab seeks to understand the life cycle of the Plasmodium parasite and identify weak points that a vaccine could target. It’s a significant undertaking, especially as the lab has recently relocated from Imperial College London to UNSW in Sydney.
“Once you have the life cycle established, then you can start looking at interventions that stop it,” Prof. Baum said.
The group recently identified the genes expressed by the Plasmodium sporozoite, a form of the parasite transmitted from the mosquito salivary gland to the host. These genes, published in Nature Communications, likely contain targets that would work as part of a vaccine.
Currently, researchers in the lab are growing parasites in a mixture of blood and cell culture medium. They are also working to establish an insectary – a tightly regulated area for breeding Anopheles mosquitos so they can be infected with Plasmodium.
When the insectary is up and running later this year, the researchers will be able to study the full Plasmodium life cycle and test experimental vaccines directly. They anticipate a ramping up of research output, including new leads for vaccine development, to contribute to the ultimate goal of malaria eradication.
"Will we see eradication in our lifetime? I hope so,” Prof. Baum said.
“I think the technology is there, if we're brave enough, and we use it well enough.”