Practice makes perfect: the importance of simulation learning in medicine
Simulation learning helps medical students and professionals to prepare for real-life situations.
Simulation learning helps medical students and professionals to prepare for real-life situations.
It takes many hands to provide patient care. In diverse settings and in sometimes high-pressure situations, medical professionals must work together in multi-disciplinary teams. Simulation learning is a valuable tool to help prepare for these experiences.
UNSW Medicine & Health continues to build simulation expertise and capabilities to support students and medical professionals to train and learn together. The South West Sydney Clinical Skills and Simulation Centre is a partnership between UNSW, the South Western Sydney Local Health District and the Western Sydney University, under the partnership umbrella of the Ingham Institute for Applied Medical Research.
Conjoint Associate Professor Ben Taylor has recently been appointed the Director of Simulation for the School of Clinical Medicine. A senior specialist in Emergency Medicine at Liverpool Hospital, A/Prof. Taylor is also an award-winning medical educator specialised in emergency and simulation teaching. Below, A/Prof. Taylor explains what simulation learning exactly is and what that looks like at UNSW.
Q: What is simulation learning and why is it important?
A: Simulation is a form of experiential learning where students, doctors and other healthcare professionals get together and practice different patient scenarios that recreate real life situations in a safe learning environment. This type of teaching is beneficial at all levels of training – from students to experienced specialists. It allows us to train in teams both for the common situations we encounter but also the rarer presentations whilst ensuring patient safety.
It’s important that the different specialties and healthcare professions train with each other. Often, healthcare professionals and students train in silos. But that doesn’t reflect what happens in real life in hospitals and in the community – where we work in multi-disciplinary teams.
Q: What does simulation learning actually look like?
A: Simulation-based learning can take place in a variety of environments, for example in a clinical setting like a hospital or outpatient clinic (in situ simulation) or purpose-built simulation teaching space. For example, the UNSW South West Sydney Clinical campus at Liverpool has a world class simulation centre which includes a variety of simulation spaces designed to be used as multifunctional rooms that can be set up as an ED resuscitation bay, an operating theatre, inpatient ward room or an outpatient clinic room.
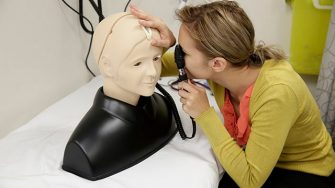
We often use a type of sim training equipment called a task trainer, which is a specialised model that helps the learner practise a specific procedural skill. This ranges from a very realistic model of a human arm to train people to insert a cannula, all the way up to advanced mannequins… These mannequins can breathe, have palpable pulses, audible heart and other body sounds, even talk with the learner.
The scenarios can range from very basic tasks like practicing examination skills for phase one students where the trainer is always in the room, to more complex immersive scenarios for more advanced students. After the simulation there is the ‘debrief’ - this is a facilitated learning conversation which gives an opportunity to sit down and ask the learners to reflect on what they learned. We talk about their experiences, what they did well, and what they could improve upon.
One of the emergency and trauma simulation labs at the South West Sydney Clinical Skills and Simulation Centre. Photo: Guy Wilkinson.
Q: What are you aiming to accomplish as the Director of Simulation?
A: My role is to help coordinate and build upon the existing simulation learning and teaching programs across the School of Clinical Medicine. I hope I can help by collaborating with all the sim educators to standardise and enhance the great stuff that is already happening in this space across all the clinical sites with the aim of elevating the student experience even more.
The field is quickly evolving – the next era will probably include innovation in virtual reality-based simulation training. So as a school we’ve been looking into how we can incorporate this technology to make simulation training more resource efficient and accessible.
I think it’s also important to say that simulation is just one teaching tool available to us – it will never replace real patient interaction. But it has great potential to enhance learning and help to train a new generation of doctors who are equipped with all the skills they need to be workplace ready on day one as an intern.
Image caption: Task trainers help medical students and professionals to practice clinical skills. Photo: UNSW.
Associate Professor Ben Taylor is the Director of Simulation for the School of Clinical Medicine. Photo: UNSW.